|
BOOK NOW |
ASK ABOUT YOUR PAIN |
Home > Blog > Physiotherapy > Milwaukee shoulder syndrome
Milwaukee shoulder syndrome
Milwaukee shoulder syndrome (apatite-associated destructive arthritis) is a rheumatological condition similar to calcium pyrophosphate dihydrate deposition disease (CPPD). It is associated with periarticular or intra-articular deposition of hydroxyapatite crystals.
Crystal deposition in the joint causes the release of collagenases, serine proteases, elastases, and interleukin-1. This precipitates acute and rapid decline in joint function and degradation of joint anatomy. Subsequently disruption of the rotator cuff ensues.
Along with symptomatology, the disease typically presents with positive radiologic findings, often showing marked erosion of the humeral head, cartilage, capsule, and bursae. Though rare, it is most often seen in females beginning in their 50s or 60s.
Diagnosis is made with arthrocentesis and Alizarin Red staining along with clinical symptoms.
Signs and symptoms
Signs and symptoms may include the following:
- Limited active range of motion, usually unrestricted passive range of movement (early)
- Joint pain
- Joint stiffness
- Joint inflammation and tenderness
- Synovial hemorrhagic effusion/hematoma
- Radiologic positive findings
- Hydroxyapatite crystals in synovial fluid
Diagnosis
Xrays, arthrography, USG, CTScan and MRI are helpful in diagnosing this condition
Treatment
Treatment may include the prescription of one or more of the following:
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Intra-articular steroids
- Physical therapy
- Partial or complete arthroplasty
Milwaukee shoulder syndrome physiotherapy
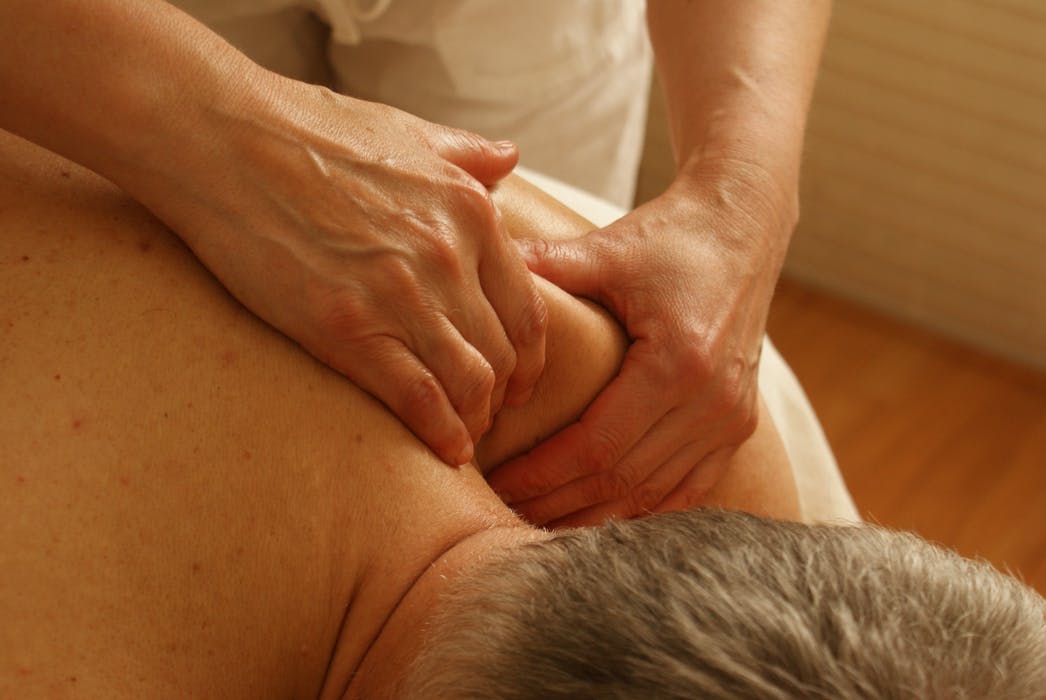
The goals of treatment are to reduce pain, decrease inflammation, and improve a person's overall functioning.
Research studies have shown that physical exercise of the affected joint can noticeably improve long-term pain relief. Furthermore, exercise of the arthritic joint is encouraged to maintain the health of the particular joint and the overall body of the person.
Individuals with arthritis can benefit from both physiotherapy and hand therapy. In arthritis the joints become stiff and the range of movement can be limited. Physical therapy has been shown to significantly improve function, decrease pain, and delay need for surgical intervention in early to advanced arthritic cases.
Exercise prescribed by a physiotherapist has been shown to be more effective than medications in treating osteoarthritis of the knee. Exercise often focuses on improving muscle strength, endurance and flexibility.
Physiotherapy intervention includes
- decreasing and managing ongoing pain and inflammation with cold therapy
- ultrasound therapy to accelerate the healing process
- joint and soft tissue movement and range of motion
- muscle strengthening of the affected joints and the muscles around it
- weight loss programs such as exercises, working with our dietitian
- prescribe any walking aids if necessary and train how to use them safely and effectively
- prescribe customized finger, hand or foot splints
We don't recommend patients take medicine or painkillers for long term due to risk of side effects as well as addictions, and for severe cases, patients may consider joint replacement surgeries. An artificial joint can last 10-15 years.
That being said, one of the best ways to treat rheumatoid arthritis is prevent it entirely by being active, and you can exercise with us and our senior physiotherapists to prescribe arthritis-specific exercises programs. If you already have it, then we can help to slow down the progress by managing it well.
Even if you require surgery, post-surgery physiotherapy will help you accelerate your progress to back to work, life and activities that matter to you.